Yes—Pregabalin can be helpful for some people with Fibromyalgia, but it’s not a perfect solution and doesn’t work for everyone. Here’s a clear, balanced explanation so you understand where it fits.
🧠 What pregabalin does
Pregabalin works by calming overactive nerve signals in the brain and spinal cord. In fibromyalgia, the nervous system is often hypersensitive, so normal sensations feel painful. Pregabalin helps reduce that “volume.”
✅ How effective is it?
It can reduce pain in some people (especially nerve-type pain)
It may improve sleep, which is a big issue in fibromyalgia
Some patients report less anxiety, which can also help symptoms
However:
It does not cure fibromyalgia
Only about 30–50% of people get meaningful relief
Benefits may take 1–2 weeks (or longer) to notice
👍 Who it works best for
Pregabalin tends to help more if you have:
Burning, tingling, or nerve-like pain
Poor sleep or frequent waking
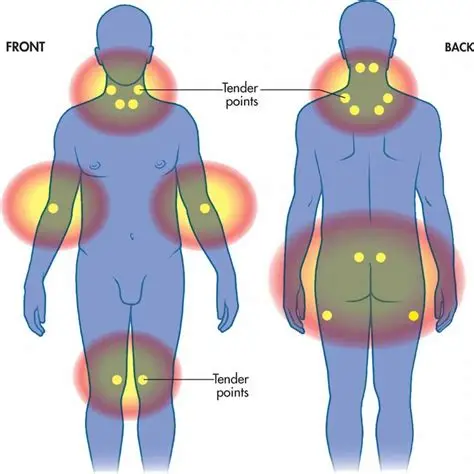
High sensitivity to touch or pressure
👎 Common downsides
Side effects are quite common, especially at the start:
Drowsiness / fatigue
Dizziness
Weight gain
Brain fog / difficulty concentrating
Swelling in hands or feet
Some people stop it because of these.
⚖️ Is it “good” overall?
Short answer:
👉 It’s good for some people, not all.
Think of it like this:
✔ Helpful tool in a treatment plan
✖ Not a standalone fix
⚠ Requires trial-and-error to see if it suits you
🧩 Best used as part of a bigger plan
Pregabalin works best when combined with:
Gentle exercise (like walking or stretching)
Sleep improvement strategies
Stress reduction (CBT, relaxation, etc.)
Other medications if needed
🚫 When it may NOT be ideal
It might not be the best choice if:
You’re very sensitive to medications
You already struggle with fatigue or brain fog
You’re concerned about weight gain
💬 Bottom line
Pregabalin is one of the main approved medications for fibromyalgia, and it can make a real difference—but it’s not universally effective.
👉 The only way to know if it’s “good for you” is a carefully monitored trial with your doctor, starting at a low dose.
If you want, I can compare pregabalin with other fibro meds (like duloxetine or amitriptyline) so you can see which might suit you better.
Yes—Pregabalin can be effective for some people with Fibromyalgia, but its benefits vary significantly across individuals, and its clinical value must be understood in a nuanced, evidence-based context.
Pregabalin is an anticonvulsant and neuropathic pain agent that modulates calcium channel activity in the central nervous system, thereby reducing the release of excitatory neurotransmitters such as glutamate and substance P. This mechanism is particularly relevant in fibromyalgia, a condition characterized by central sensitization—where the brain and spinal cord amplify pain signals.
From a clinical standpoint, pregabalin has demonstrated efficacy in reducing pain intensity, improving sleep quality, and, to a lesser extent, enhancing overall quality of life in fibromyalgia patients. It is one of the few medications specifically approved for fibromyalgia treatment in several countries, including by the U.S. Food and Drug Administration.
However, its effectiveness is not universal. Clinical trials and real-world data indicate that only a subset of patients—often estimated around 30–50%—experience meaningful pain relief. For others, the benefits may be minimal or outweighed by adverse effects.
Common side effects include dizziness, somnolence, weight gain, peripheral edema, and cognitive blunting (often described as “brain fog”). These effects can limit tolerability, particularly at higher doses. Additionally, pregabalin carries some risk of dependence or misuse, especially in individuals with a history of substance use disorders, although this risk is generally lower than that of opioids.
In therapeutic practice, pregabalin is typically introduced at a low dose and titrated gradually to balance efficacy and tolerability. It is often used as part of a multimodal management strategy that includes non-pharmacological interventions such as exercise therapy, cognitive behavioral therapy, and sleep optimization.
Comparatively, other pharmacologic options for fibromyalgia include serotonin-norepinephrine reuptake inhibitors such as Duloxetine and Milnacipran, as well as low-dose tricyclic antidepressants. The choice among these depends on symptom profile, comorbidities, and patient-specific response patterns.
In summary, pregabalin can be “good” for fibromyalgia in a subset of patients—particularly those with prominent sleep disturbance and neuropathic-type pain—but it is not a universally effective solution. Its use should be individualized, closely monitored, and integrated into a broader, multidisciplinary treatment plan.